CHIARI MALFORMATION
General Information, Symptoms and Treatment
THE INFORMATION BELOW IS GENERAL EDUCATIONAL CONTENT ABOUT CHIARI MALFORMATION AND MAY NOT APPLY TO EVERY PATIENT. FOR THE MOST ACCURATE ADVICE, PLEASE CONSULT YOUR NEUROSURGERY SPECIALIST.
What Is Chiari Malformation?
Chiari malformation Type 1 is a condition in which the lower part of the cerebellum (the cerebellar tonsils) extends downward through the opening at the base of the skull into the upper spinal canal. This usually happens because the space in the back of the skull is relatively small for the surrounding neural structures.
In many patients, Chiari malformation is congenital and may remain asymptomatic for years. It is often detected incidentally on MRI scans performed for unrelated reasons, such as after a fall, accident or trauma. This incidental finding can understandably cause major anxiety in families. Importantly, not every Chiari finding requires surgery.
There are multiple Chiari subtypes. In daily clinical practice, the most common presentation in adolescents and adults is Chiari Type 1, which is the form addressed on this page.
Although many patients have no symptoms, possible complaints may include:
- Occipital headache (pain in the back of the head)
- Balance problems or gait instability
- Numbness or tingling in the hands or feet
- Difficulty swallowing
- Snoring or sleep-related breathing symptoms
- Nasal regurgitation of liquids in selected cases
- Neck or back pain
- Scoliosis in some pediatric patients
None of these findings are specific to Chiari malformation alone. Similar symptoms can occur in many other conditions, so diagnosis should be based on clinical examination together with imaging findings.
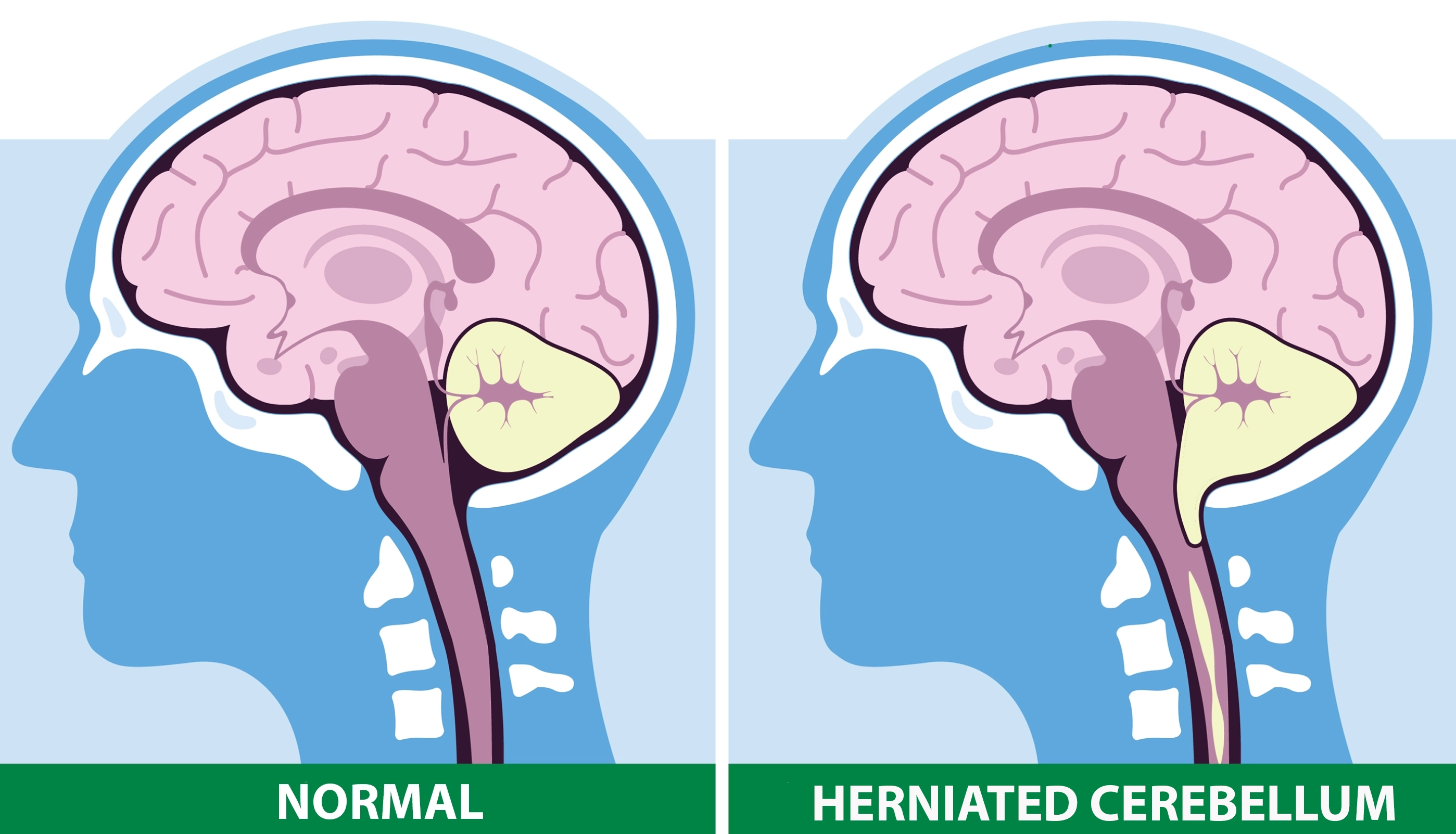
Does Every Chiari Malformation Require Surgery?
In short: no. Not every patient needs surgery. A Chiari finding on MRI alone is not an automatic indication for an operation.
First, the degree of descent matters, but treatment decisions are not based on millimeters alone. We treat patients, not MRI measurements in isolation. A patient with tonsillar descent but no meaningful symptoms or neurological findings may be followed clinically.
Second, symptoms must correlate with the diagnosis. For example, neck or occipital pain may arise from cervical disc disease, arthritis, muscle disorders, high blood pressure, or other common causes. Surgery is considered when symptoms cannot be explained better by another cause and are truly attributable to Chiari pathology.
Third, neurological examination findings are important. Dizziness, balance problems, gait disturbance, weakness or sensory loss in the hands or feet, and reduced gag or swallowing reflex may support a surgical indication.
Finally, MRI is evaluated for associated findings such as disrupted cerebrospinal fluid (CSF) flow at the junction of the skull and neck or syringomyelia (a fluid-filled cavity within the spinal cord), which can strengthen the indication for decompression surgery.
Overall, treatment decisions are individualized after comprehensive review of symptoms, examination, and imaging.
Is Chiari Malformation a Serious Disease?
In most people, Chiari malformation does not cause a serious problem and does not require surgical treatment.
The symptoms described above appear in a smaller group of patients, and surgery is considered for selected patients in that group.
Is Chiari Malformation Surgery a Major Surgery?
No operation is "minor" for the individual patient. Every procedure has potential risks and benefits that should be discussed in detail.
In general, posterior fossa decompression for Chiari is not as complex as some other neurosurgical operations, such as many brain tumor surgeries, but it still requires experienced surgical planning and follow-up.
What is done in surgery?
The operation begins with a midline incision at the back of the neck, and the tissues are exposed up to the skull bone.
The main goal is to relieve the area where the cerebellum is crowded. For this purpose, a small piece of bone is removed from the part of the skull near the neck.
In most cases, the membrane around the brain and spinal cord is opened and widened with a patch. This gives the cerebellum more room to move freely within the skull.
Chiari Malformation Surgery
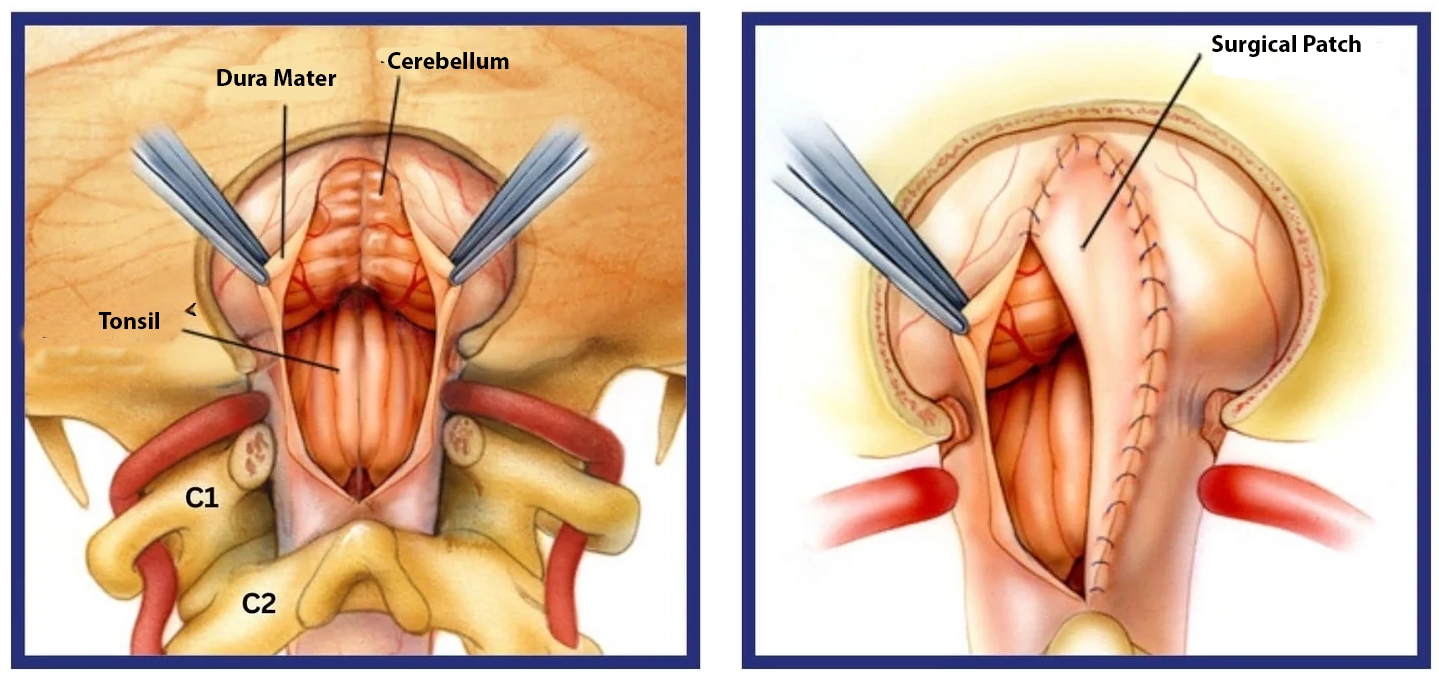
Are Chiari Malformation Surgeries Successful?
These operations were described long ago and have been performed safely for many years. After surgery, complaints decrease or disappear completely in many patients. Therefore, these operations are generally considered successful.
However, it should be remembered that, like any surgical method, it is not perfect and cannot be successful in one hundred percent of patients.
Many factors, especially the patient's age and underlying causes, affect surgical success. The first goal of surgery is to prevent the problem from progressing. In many patients, complaints decrease after surgery or may even disappear completely. If there is a fluid-filled cavity in the spinal cord, it may also shrink. In some patients, however, complaints do not fully resolve or new complaints may appear. These situations are often temporary and improve over time.
It is important to remember again that the patient's well-being is what matters most. In some patients, imaging may not show complete improvement, but the patient's complaints improve; for these patients, surgery is considered successful.
In very rare cases, the procedure may not achieve the expected result and the patient's complaints or radiological imaging may worsen. In such cases, different treatments or even additional surgery may be considered.
As a result, Chiari malformation surgery can be a very successful surgical intervention. However, each patient must be evaluated individually and the treatment plan should be made accordingly.
Frequently Asked Questions
If the membrane around the brain and spinal cord was opened and closed with a patch during your surgery, the most important problem you may encounter is cerebrospinal fluid leakage from this patch. Most cases can be managed with pressure dressings and wound care, but sometimes a second operation may be needed to repair the leaking area. Apart from this, as with any surgery in this region, neck muscle pain and limited movement are common, but these usually improve with time and good pain control.
The answer is most likely no. In some patients, cerebellar tonsillar descent may become less prominent with growth and age. In children, follow-up is often recommended until growth and development are complete. Therefore, if your doctor says surgery is not needed right now, you will probably not need surgery later either. However, this does not apply to every patient, and some patients may need surgery at a later age. For this reason, it is important to follow your doctor's recommendations.
Unfortunately, this is not a question that can be answered easily for everyone. Many people live normal lives without ever being diagnosed, and pregnancy and delivery may occur in such patients. The most appropriate approach should be clarified through a joint decision by obstetricians and neurosurgeons.