Cervical Disc Herniation
General Information, Symptoms and Treatment
Prof. Dr. Alp Özgün Börcek at Ankara Güven Hospital provides diagnosis and treatment for cervical disc disorders within pediatric and adult neurosurgery and spine surgery practice. The information on this page is general and does not replace an in-person medical evaluation.
THE INFORMATION BELOW IS GENERAL EDUCATIONAL CONTENT ABOUT CERVICAL DISC HERNIATION AND MAY NOT APPLY IDENTICALLY TO EVERY PATIENT.
NECK PAIN CAN HAVE MANY CAUSES OTHER THAN HERNIA AND THESE SHOULD BE INVESTIGATED.
FOR THE MOST ACCURATE DIAGNOSIS AND TREATMENT PLAN, PLEASE CONSULT A NEUROSURGERY SPECIALIST.
Which Department to Go to for Neck Pain?
Patients with neck pain may initially consult either Neurosurgery or Physical Therapy and Rehabilitation . In routine practice, surgery for cervical disc herniation is generally performed by neurosurgeons, while physical therapy teams focus on conservative management such as exercise, rehabilitation, and medication-based pain control. The appropriate referral depends on symptom severity, duration, and neurological findings.
What causes neck and arm pain?
Problems originating from the neck can cause arm pain through the nerves and muscle structures extending from the shoulder to the hand. Posture disorder, nerve compression or muscle spasm are among the most common causes. The following list summarizes the causes most often seen in clinical practice.
- - Prolonged poor posture (desk, phone use)
- - Cervical disc degeneration or herniation
- - Nerve root compression (cervical radiculopathy)
- - Muscle spasm and myofascial pain syndrome
- - Shoulder joint pathologies (frozen shoulder, rotator cuff tear)
- - Nerve entrapments (carpal tunnel, cubital tunnel, etc.)
- - Thoracic outlet syndrome
- - Rheumatic diseases (ankylosing spondylitis, RA)
- - Trauma or sudden neck strain (whiplash)
- - More rarely: infection, tumor, metastasis
What Is Cervical Disc Herniation?
Cervical disc herniation occurs when disc material between the neck vertebrae protrudes beyond its normal boundary. The protruding disc may compress a nerve root or, in more advanced cases, the spinal cord. This can cause neck pain, radiating arm pain, numbness, tingling, or weakness.
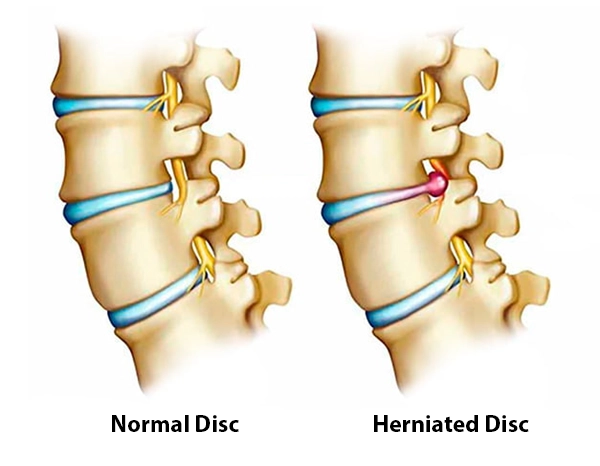
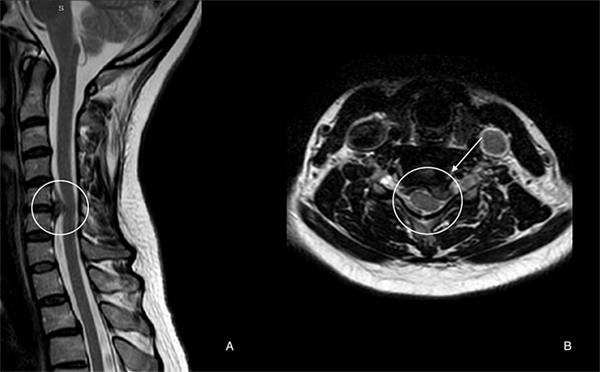
Why does our neck hurt?
Discs wear out and lose elasticity over time. This can lead to tears in the outer layer of the disc. The soft inner structure may protrude outward and compress the nerves. This compression can irritate the nerve root through both chemical and mechanical effects.
The main reason is that the human spine wears over time through natural processes, much like skin wrinkling or hair turning gray.
NECK PAIN DOES NOT ALWAYS MEAN A DISC HERNIATION OR A SPINAL PROBLEM.
What matters is the type and duration of the pain and whether it responds to painkillers, massage, appropriate exercises or rest.
Pain can sometimes be very severe, but the underlying cause does not have to be a disc herniation. Most neck pain improves without treatment or with simple treatments. Neck pain requiring surgery is relatively rare.
What Are the Symptoms of Cervical Disc Herniation?
- Neck pain
- Pain radiating along the shoulder, arm or hand (radiculopathy)
- Numbness, tingling
- Decreased muscle strength
- Reduced reflexes
- Rarely, gait disturbance due to spinal cord compression and instability (myelopathy)
When should you consult a doctor for neck pain?
First of all, it is important to note that your pain if you are worried, you can consult a doctor at any time. A physical medicine specialist, neurosurgeon or family doctor can help.
Beware of Red Flags!
If your complaints include weakness in the arm or hand, imbalance, or difficulty walking,
If your pain does not improve with simple painkillers, increases despite rest, or appears especially at night and wakes you from sleep,
If your neck pain started after a fall or accident,
If your pain is accompanied by fever,
If you have a known cancer and neck pain is new has started, accompanied by unplanned weight loss,
If you use cortisone (steroid) medicines for a long time or at high doses and have new neck pain,
YOU SHOULD DEFINITELY CONSULT A SPECIALIST DOCTOR.
How Is Cervical Disc Herniation Treated?
Treatment of cervical disc herniation depends on disease severity and how much the patient's quality of life is affected. In the first stage, rest, physical therapy and medications are usually sufficient. Strengthening the neck muscles with exercise is very effective in the long term. In more advanced cases, injection treatments or surgery may be considered. The treatment process is individualized, and the best approach should be determined after evaluation by a specialist.
Cervical Disc Surgery
Cervical disc herniation surgeries have been performed successfully for many years and are reliable methods. In most patients, surgery is performed through an incision on the front of the neck, as shown below. In rare cases, if spinal cord compression is greater from the back, a posterior approach may be used. During surgery, the herniated disc tissue is removed and pressure on the nerve root is relieved. This procedure is performed under general anesthesia, and patients are usually discharged the next day.
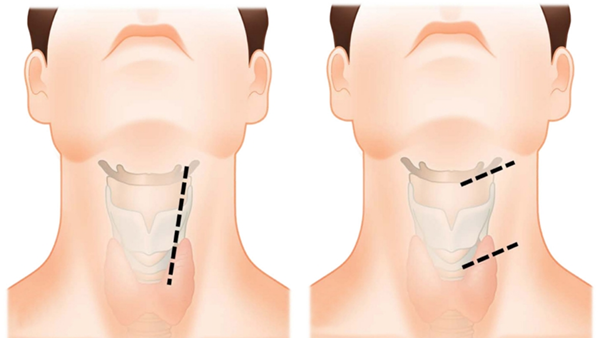
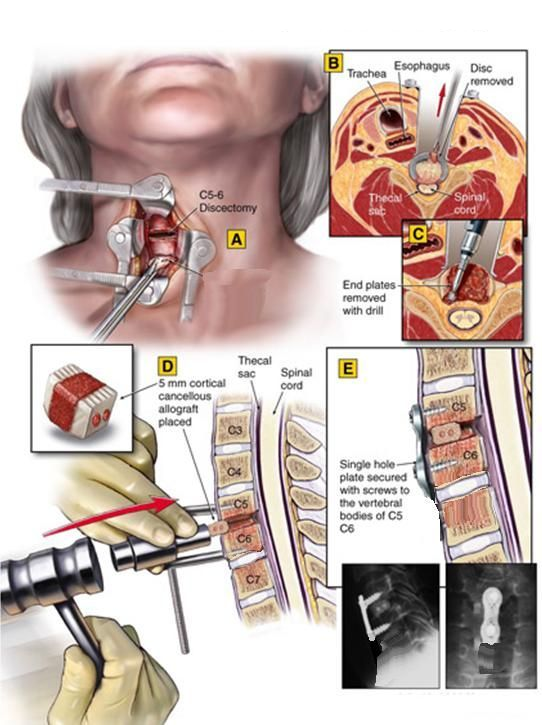
After surgery, patients are helped to stand as soon as possible and are encouraged to return gradually to daily life...
What Is the Difference Between Cervical and Lumbar Disc Surgery?
Lumbar disc herniation surgeries are often misunderstood by the public and therefore feared more than necessary. People often act on hearsay or on negative experiences reported by a relative or acquaintance. However, every patient is different and every treatment plan is individualized.
"People are usually even more afraid of cervical disc surgery."Simple, single-level cervical disc surgeries are generally less invasive than lumbar disc surgeries and usually allow recovery in a shorter time. Patients often return to normal activities more quickly after cervical disc surgery. The most important reasons are:
- The neck carries less weight than the low back
- Cervical disc surgeries are more physiological procedures and result in less tissue damage
- Performing the operation from the front is a major advantage. Because the herniated disc tissue can be cleaned completely, the probability of recurrence at the same level is close to zero.
Frequently Asked Questions
The risk of paralysis in cervical disc surgery is very low, but in very advanced diseases that cause severe spinal cord compression - conditions beyond a simple cervical disc herniation - this risk may increase. What patients often overlook is that, in selected severe cases, not having surgery may also increase the risk of paralysis.
Apart from these exceptions, complete paralysis due to a simple one- or two-level cervical disc herniation is almost impossible.
As mentioned earlier, paralysis from a simple cervical disc herniation is extremely unlikely.
However, some patients have a more complex condition than a simple disc herniation. Degenerative thickening or ossification of tissues around the spinal canal can cause spinal cord compression (cervical myelopathy). In this situation, pressure on the cord may persist and treatment planning is more complex than routine cervical disc surgery. Surgical risk can be higher than in uncomplicated cases, although severe complications remain uncommon in experienced hands.
The main reason is anatomy. In the lumbar region, except for the uppermost part, the spinal canal contains nerve roots that are more mobile and often tolerate surgical manipulation better. In the neck, however, the spinal canal is occupied by the spinal cord itself. Therefore, cervical disc surgeries require more attention and care than lumbar disc surgeries because the spinal cord is more sensitive than nerve roots.
Please remember that this situation is no longer a simple cervical disc herniation problem; it is a much more serious disease. Your doctor will give you detailed information about it.
The answer involves many genetic and environmental factors and is a broad topic. The most basic reason, however, is increasing structural wear in the spine over time. Just as our skin wrinkles or our hair turns white with age, the spine also wears through natural processes.
In addition to natural aging, excess weight, a sedentary lifestyle, repeatedly lifting heavy weights in an unbalanced way and some metabolic diseases may contribute to cervical disc herniation.
REMEMBER: Disc herniation is not the only cause of neck pain. Consulting a specialist for correct diagnosis and appropriate treatment is extremely important.
As mentioned earlier, disc herniations are often the result of natural wear that develops in the spine with age. Findings described as "herniation" in MRI reports often reflect this aging process on imaging.
Especially from the 20s onward, disc herniation or herniation-like changes may be seen on MRI in many people. However, many of these findings are part of the normal aging process and are often not directly related to the patient's complaints.
Therefore, it is not correct to say "you need surgery" by looking only at the MRI report. What matters is whether the imaging findings match the patient's clinical condition. The person who will evaluate this is your doctor.
PLEASE REMEMBER: We treat patients, not MRI films. Although your report may contain numerous findings, in most cases, surgical treatment may not be needed.
Although repeat surgery can be an important issue after lumbar disc surgery worldwide, this is very unlikely for cervical disc herniation. Cervical disc herniation can usually be treated successfully with a single operation.
Cervical disc surgeries are generally safe procedures with a low complication rate. However, as with every surgical intervention, there are some risks.
The most common risks include infection, pain at the incision site, irritation of nerve tissue and, rarely, nerve damage. Much more rarely, bleeding or cerebrospinal fluid (CSF) leakage may occur.
One complication specific to cervical disc surgery is movement or displacement over time of the artificial disc or cage placed after the herniated disc is removed. This is very rare, but if it occurs, another operation may be needed to reposition the material.
Pain may continue for a while after cervical disc surgery, and this is usually considered normal. Temporary pain, tingling or numbness may occur while the nerve tissue and surrounding tissues heal.
These symptoms usually decrease over time. However, if your pain is very severe, increasing, or lasting longer than expected, you should consult your doctor. In some cases, persistent severe pain may be a sign of an additional problem or complication.
To put it plainly, if a cervical disc herniation is truly causing a problem that requires surgery, there is unfortunately no equivalent non-surgical treatment for that mechanical problem. A disc herniation means tissue is present where it should not be and is causing pressure. In that situation, the definitive treatment is to remove the herniated tissue mechanically, that is, surgically.
However, as explained above, not every disc herniation requires surgery. In most patients, painkillers, cervical collar use and physical therapy methods are enough to improve pain and quality of life. Surgery is an exceptional decision made after considering many different findings.